The monitoring of type 2 diabetes using urine testing relies on the renal threshold for glucose being around 10 mmol/l, so that as soon as the renal threshold is exceeded, glucose begins to be excreted by the kidneys and is picked up by a chemical enzymatic reaction on a testing strip (Fox and Pickering, 1995).
As good control of diabetes would never result in the renal threshold for glucose being exceeded, then good control is indicated if no sugar is detected. Thus, people with diabetes should be advised that their goal in self-monitoring of urine glucose (SMUG) is to never find glucose and to take action if they do.
Its main advantage
Two key advantages of SMUG are that it is non-invasive, and, compared with self-monitoring of blood glucose (SMBG), cheap: urine test strips range from £2.26 to £3.25 for 50 whereas blood test strips range from £13.15 to £15.87 for 50 on the NHS drug tariff (The NHS Electronic Drug Tariff, 2006).
Disadvantages
Disadvantages of SMUG include that urine glucose tests cannot detect hypoglycaemia. Also, individual renal thresholds for glucose can vary, so some people excrete glucose when at a normal blood glucose level, while some do not excrete glucose even at very high levels (Graham, 1926). There is no routine test to establish an individual’s renal threshold for glucose, so it has to be determined by deduction: if the HbA1c does not correlate with the individual’s urine glucose test results, for example. In these circumstances, the author would usually get him or her to monitor their blood glucose at the same time as urine testing for a couple of weeks to compare the results.
Another problem is that even if the renal threshold for glucose is normal, an individual could have blood glucose levels between 8 and 9.9 mmol/l and from their consistently negative urine tests mistakenly believe his or her diabetes was under control.
Practical limitations
SMUG test results reflect occurrences in the blood from several hours previously. Thus, it cannot be used to make safe insulin dose adjustments. People often relate raised urine glucose to food eaten immediately before the test was taken – food that has not entered the blood stream as glucose yet, let alone been excreted by the kidneys.
Also, people like to ‘see’ something when they test, and a frequent reason cited for stopping testing is ‘it never showed anything’, even though they have been told this is their goal (Lawton et al, 2004). In addition, although this method of testing is non-invasive, some people do not like handling urine or find the test fiddly or difficult to perform. Because SMUG relies on visual colour difference determination, the educator needs to check that the patient can see the differences in test strip colours before allowing them to urine test independently.
There are also some test interferences that give false negatives, such as vitamin C, aspirin, iron supplements, levodopa and tetracycline-type antibiotics. The strips deteriorate on exposure to air so correct storage and observation of expiry dates are also important.
When to test
Patients should be advised to test their urine at different times during the day because blood glucose levels fluctuate. If someone always tests at the same time each day they may gain a false picture of their level of control.
How to test
The reagent pad on the strip should be dipped into a fresh sample of urine and removed immediately. Any excess urine should be wiped off against the side of the sample container. The tester should then time the exact number of seconds recommended by the manufacturer (this usually ranges between 30 and 60 seconds) from the time the strip comes into contact with the urine. The colour on the reagent pad should then be compared against the manufacturer’s chart. The result should be recorded by the individual on his or her monitoring chart.
In theory, the patient could place the strip in the urine stream when they pass urine but this would mean monitoring the time and holding the bottle to compare the strip colour simultaneously, which in practice is not easily achieved.
Risk of hypoglycaemia
Guidelines published in 2004 recommend that people on sulphonylureas or insulin should not use SMUG because of the associated risk of hypoglycaemia (Owens et al, 2004). However, in the author’s experience, most people with diabetes taking sulphonylureas do not routinely self monitor their blood glucose.
Ketones
The other use of urine testing in people with diabetes is to detect ketones. There are test strips which determine the amount of ketones in urine, and everyone with type 1 diabetes should know when and how to test for ketones and what action to take if any are found. There are blood ketone test strips available and some diabetes care centres recommend these instead of the urine test strips.
Conclusion
Urine testing for glucose can be effective if used properly and is still widely used as a monitoring method. A study carried out in the author’s centre found no difference between levels of control after 3, 6 and 12 months in people recently diagnosed with type 2 diabetes who used SMUG and those who used SMBG (Miles et al, 1997). However, participants expressed a preference for blood glucose monitoring as they perceived it to be more accurate and useful in self-management (Miles et al, 1997). If urine testing is being used as the monitoring method, regular checks of HbA1c need to be carried out to ensure that adequate control is being achieved.
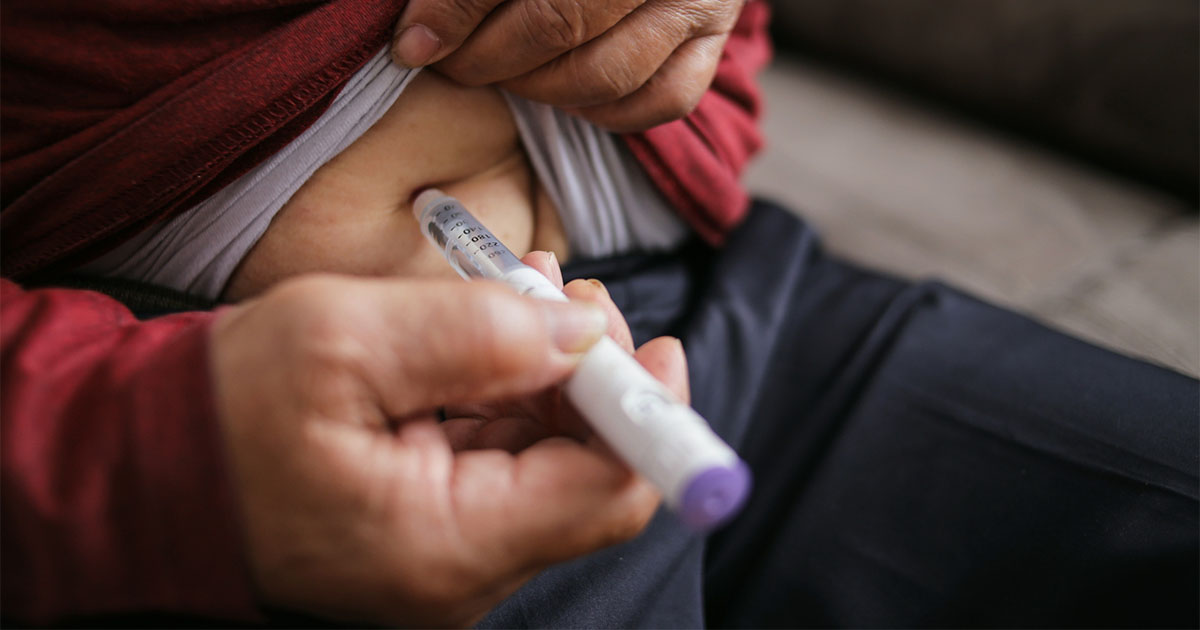
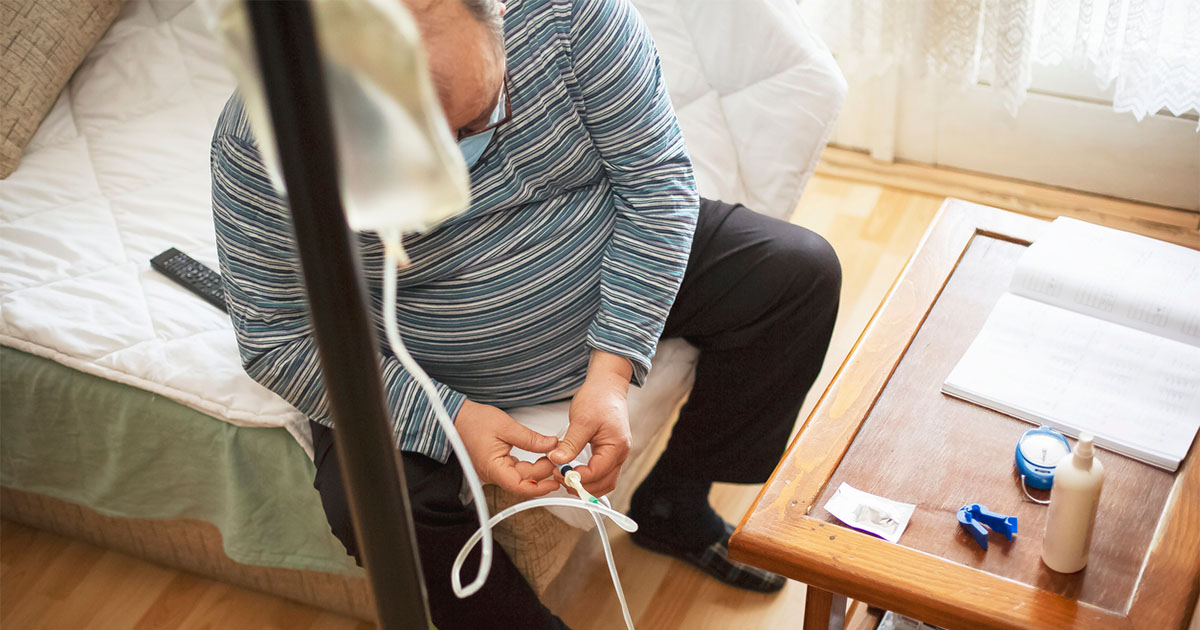


No strong support for weight cycling causing detrimental changes in body weight, body composition or metabolism, but many gaps in the research.
5 Jun 2026