| Article key points |
| 1. Obesity is a complex long-term condition, requiring holistic, person-centred care. 2. Access to tirzepatide (Mounjaro®) for the management of obesity in primary care is prioritised on the basis of clinical need, ensuring that those at greatest risk of obesity-related complications are supported first. 3. A new Quality and Outcomes Framework indicator will support practices to offer assessments and treatment to all eligible people within the clinically prioritised cohorts, helping to embed a systematic approach to care, while supporting implementation of the wider pathway. 4. NICE guidance, MHRA licensing and NHS England commissioning guidance require that tirzepatide should not be used as a standalone treatment; it should be accompanied by diet and activity modification supported by a structured behavioural intervention. 5. In this context, “Wraparound care” includes both clinical management and structured behavioural support. 6. Integrated Care Boards determine whether behavioural support is provided through national or locally commissioned services, but in all cases this support should be accessible and aligned with prescribing. |
General practice plays an essential role in supporting the developing clinical pathway for obesity and weight management, helping to ensure people with the greatest clinical need can access appropriate care in a fair and equitable way. General practice teams are recognised for their expertise in delivering holistic, person-centred care and their deep understanding of their patient populations. This places them in a strong position to recognise when additional support may be needed, and to guide patients through coordinated, individualised weight management pathways.
Evolution of weight management pathways
The publication of the NICE (2024) Technology Appraisal for tirzepatide (Mounjaro®) for the management of obesity, alongside its phased implementation by the NHS through a NICE Funding Variation, has marked an important step in the evolution of weight management in primary care.
As a result, general practice teams are developing their experience of managing obesity as a long-term condition within an emerging holistic clinical care pathway. This approach reflects a shift towards treating obesity in a similar way to other chronic conditions, with structured assessment, ongoing management and continuity of care. Eligibility criteria based on BMI and weight-related comorbidities help ensure that access to treatment is grounded in clinical need, supporting a consistent and visible approach across patient populations.
The introduction of Quality and Outcomes Framework (QOF) indicators for weight management in the 2026/27 GP contract (NHS England, 2026a) further supports this shift. By encouraging practices to assess people within the clinical cohorts prioritised by NHS England (2026b), QOF will provide a structured mechanism for case finding and engagement, helping to move from more opportunistic approaches towards a proactive, population-based model of care.
At the same time, both the NICE Technology Appraisal and the MHRA licence make clear that tirzepatide for the management of obesity is not intended to be used in isolation. These recommendations from regulators are underpinned by evidence from clinical trials that required the medication to be delivered alongside structured behavioural and lifestyle support.
While many practices have begun to develop confidence in how these elements work together in routine care, discussions with GPs across England suggest that some uncertainty remains about what the pathway requires in practice. In particular, the concept of “wraparound care”, and how it should be implemented alongside prescribing, can feel unclear.
The importance of wraparound care
NHS England defines wraparound care as comprising two complementary components: clinical support and behavioural support, which together form a single, integrated approach to treatment.
Clinical wraparound care is delivered by the prescribing healthcare professional or service, and includes comprehensive assessment to confirm eligibility according to the NHS priority cohorts (NHS England, 2026b); safe initiation in line with NICE (2024) criteria; and dose titration. Regular monitoring is recommended to manage side effects, address potential drug interactions, manage related long-term conditions (including adjusting concurrent medications where appropriate), assess progress and determine whether treatment remains clinically appropriate.
Behavioural wraparound care focuses on helping people develop sustainable dietary, nutritional and physical activity behaviours alongside medication. This is delivered through structured, evidence-based behaviour change approaches, tailored to the individual receiving obesity pharmacotherapy.
Importantly, behavioural support is designed to complement, not replace, clinical care. As such, behavioural support plays a key role in helping people to make and sustain changes that support not only weight loss, but also long-term weight maintenance and wider health and wellbeing.
How behavioural and clinical support work together
Wraparound care describes the alignment of both the clinical and behavioural change support elements of the same pathway. Behavioural support provides people with the knowledge, skills and confidence to understand and make sustainable changes, while clinical support ensures safe and effective clinical oversight for the use of medication and appropriate management of comorbidities.
In practice, this means behavioural support is delivered as part of the overall treatment pathway and includes reinforcing the importance of engaging with both behavioural and clinical elements of care. Clinical support, in turn, includes prescribing responsibility, eligibility assessment and ongoing medical management, while continuing to emphasise the value of behavioural support.
Behavioural sessions may be delivered by appropriately trained non-clinical staff, whereas overall clinical management is overseen by an appropriate healthcare professional, such as a GP or specialist prescriber. Clinical teams, therefore, retain responsibility for assessing eligibility for tirzepatide for the management of obesity, considering individual factors and determining whether primary care prescribing is appropriate or whether referral to specialist services may be required.
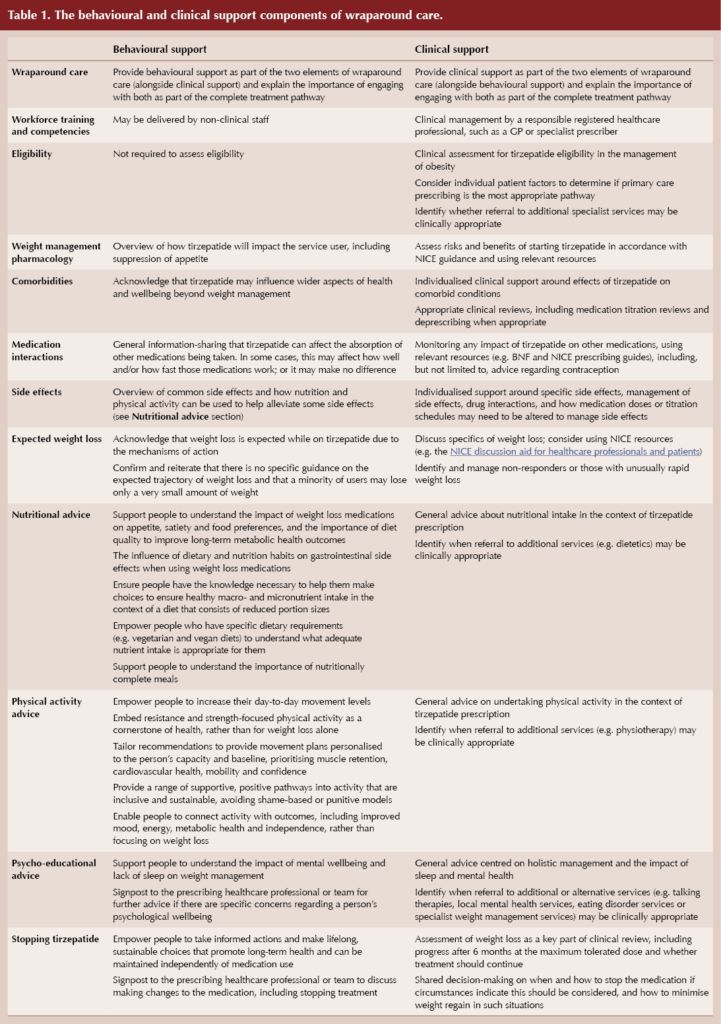
Within this model, patients receive consistent and complementary support. Behavioural and clinical support elements function as interdependent parts of a single, integrated pathway, experienced by the individual as one package of care rather than separate, optional components. The features of behavioural and clinical support are set out in more detail in Table 1.
Behavioural support helps people understand the effects of tirzepatide, including its impact on appetite and satiety, while clinical teams support shared decision-making and provide oversight of risks and benefits, in line with NICE guidance. Similarly, behavioural interventions acknowledge the wider impact of treatment on health and wellbeing, while clinical care focuses on the active management of comorbidities, including medication review, titration and deprescribing where appropriate.
This complementary approach extends to medication safety and side effect management. In behavioural support, people are supported to understand potential interactions and common side effects, while clinical teams take responsibility for monitoring, managing interactions and adjusting treatment where needed. Expectations around weight loss are also addressed jointly, with behavioural support helping people understand variability in response, and with clinical teams monitoring progress and identifying where further review may be required.
Nutritional, dietary, physical activity and wider educational support form a core part of behavioural interventions, helping people build sustainable habits and improve overall wellbeing. Clinical teams reinforce this approach through general advice and, where appropriate, identify when referral to additional services, such as dietetics, physiotherapy or mental health support, may be appropriate.
Primary care is central to making this work in practice, with GP teams bringing a deep understanding of their patients, continuity of care and expertise in managing complex long-term conditions. This places them in a uniquely strong position to coordinate care, personalise treatment decisions, and ensure that clinical and behavioural elements come together in a way that is genuinely person-centred.
Access to behavioural support
All people prescribed tirzepatide in primary care for the management of obesity in line with the NICE Funding Variation cohorts and NHS commissioning guidance should be offered access to structured behavioural support as part of their care. To enable this, NHS England has commissioned a universal behavioural support offer, available to all eligible patients, free at the point of access and centrally funded.
This national service, the NHS Behavioural Support for Obesity Prescribing (BSOP) programme, ensures that primary care teams can refer people into a consistent and accessible support offer, without the need for local commissioning arrangements to be in place.
Some Integrated Care Boards (ICBs) may commission local behavioural support services tailored to their populations. The national BSOP service is designed to complement these local pathways, providing a consistent baseline of support for all users while allowing flexibility where enhanced or specialist local services exist. ICBs are able to provide guidance on how behavioural support is delivered within their area and how referrals should be made.
The BSOP service provides nine months of structured behavioural support, available digitally, remotely or in person, allowing users to choose the format that best suits their circumstances and needs.
This offer is aligned with prescribing in primary care under the NICE Funding Variation. As such, people receiving treatment through specialist weight management services will continue to receive behavioural and clinical support within those services, whilst individuals accessing weight loss medications through private providers are expected to receive appropriate wraparound support as part of the care delivered by those providers.
Currently, the offer is designed to support the prescribing of tirzepatide in primary care for the indication of obesity only. People with type 2 diabetes alone, or other long-term conditions, are not yet eligible to access the wraparound care unless they also meet the Funding Variation eligibility criteria for obesity prescribing.
As eligibility expands with the phased implementation of the NICE Funding Variation, increasing numbers of people will become eligible for tirzepatide and wraparound care support. The BSOP service allocates capacity to ICBs based on anticipated need, with provision increasing in line with cohort expansion.
Conclusions: Delivering integrated weight management in primary care
Primary care teams are uniquely placed to provide holistic, person-centred care. Their expertise in managing complex, long-term conditions, combined with continuity of care and a deep understanding of their patient populations, enables them to tailor interventions and coordinate support in a way that is both clinically appropriate and sustainable.
For people prescribed tirzepatide for the management of obesity in primary care, the national behavioural support offer through the NHS Behavioural Support for Obesity Prescribing service provides a consistent and accessible foundation for wraparound care. This offer is specifically aligned to the NICE Funding Variation cohorts and complements local services where these exist, supporting the safe and effective use of pharmacotherapy within a structured pathway.
Taken together, this expanding range of treatment options, alongside targeted behavioural support for those receiving obesity pharmacotherapy, provides general practice with a stronger and more coherent “toolkit” to help people achieve meaningful and lasting improvements in their health.





Kidney Failure Risk Equation does not take into consideration ethnicity and competing risk of death. What are the implications of this?
25 May 2026