When feeling unwell for a long period of time there is always initial relief to know that the diagnosis given by your doctor is treatable. Diabetes is no exception, and in my own case I very quickly realised that the complaint would have certain restrictions.
Having type 2 diabetes, the regimen of diet, exercise, and oral medication accompanied by regular check-ups did not seem too great an imposition for a return to normality and feeling ‘well’ again. There was always the thought at the back of my mind, however, that one day the condition might worsen and I would need to treat my diabetes by injection of insulin. I do not have a phobia about needles but the thought of having to adjust to a more restrictive method of medication was not a comforting one.
Changing from oral mediation to insulin injections
In my own case my diabetes was diagnosed at the age of 39 (I am now 54), and I controlled the condition satisfactorily with diet and oral medication for approximately 10 years, after which my glycaemic control deteriorated and my consultant decided that the time had arrived when I would need to have regular injections of insulin.
I was given very little time to even consider or contemplate the doctor’s decision, having been passed immediately to the unit’s diabetes specialist nurse, who carefully explained what the new regimen of medication would involve. I was given a pen device, some simple publications to read and a prescription for insulin and needles which I obtained the same day. The diabetes nurse arranged to make a house call the next day to show me how to inject and to explain to my wife and myself how to deal with insulin successfully. We were fortunate to have the support of an excellent team at our local hospital in Llandough, Vale of Glamorgan, headed by Professor David Owens. The diabetes nurse was available for advice for most of the working day, which was a great comfort to myself – and in particular to my wife and immediate family who also wanted to know how to cope with adverse effects of the medication.
Learning to use an injection pen device
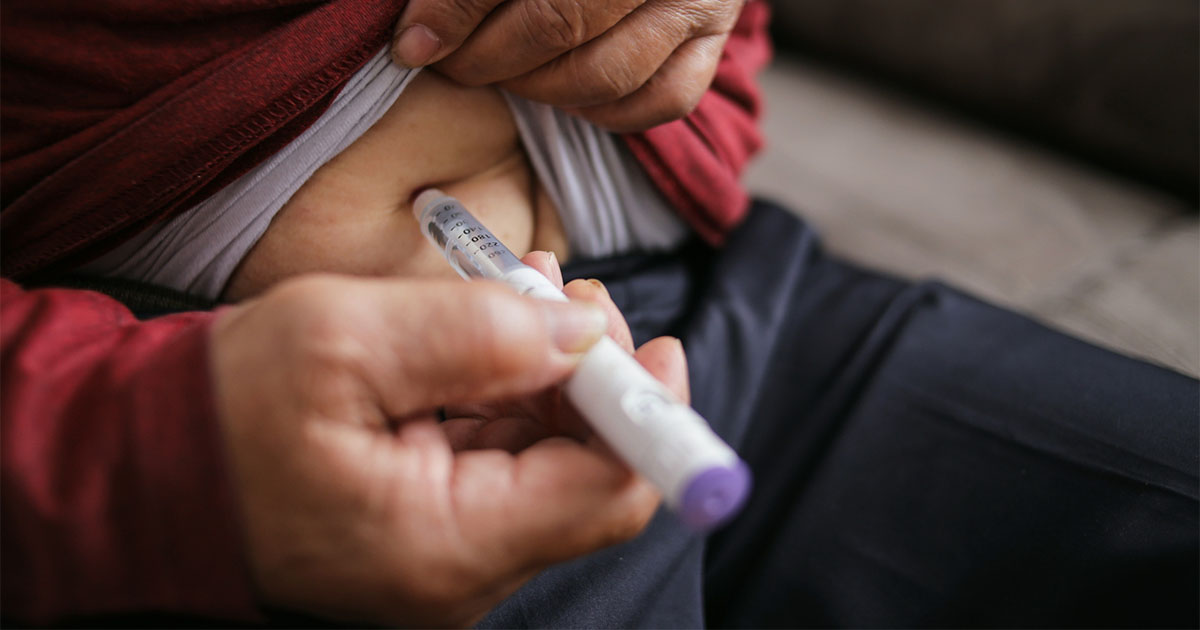
My initial concern with injecting was naturally pain and a dislike of needles, but this was not really the main issue of this form of treatment. I had spoken to other people treated with insulin who told me that the needles were very fine and could not be felt when puncturing the skin. I quickly realised that the needles provided with the pen devices were extremely fine and of different lengths to suit each individual. Provided the instructions were followed and the needles changed for each injection, then there was little difficulty with the method of delivering the insulin. The pen devices are simple to use, being easily calibrated for the dose required, and can be accommodated in a pocket or bag in the same way as a pen.
Having carried out my first injection successfully the daily routine of injections was not really a problem. The diabetes nurse actually assisted with the first injection and made the event quite relaxed. Rather than dwell on the subject of injecting, her approach was to encourage me to complete the initial injection quickly, which was proof in itself that there was no pain or inconvenience. The diabetes nurse advised on the rotation of injection sites as over-use of a site may result in poor absorption of the insulin leading to a change in glycaemic control.
Measuring blood glucose and managing hypoglycaemia
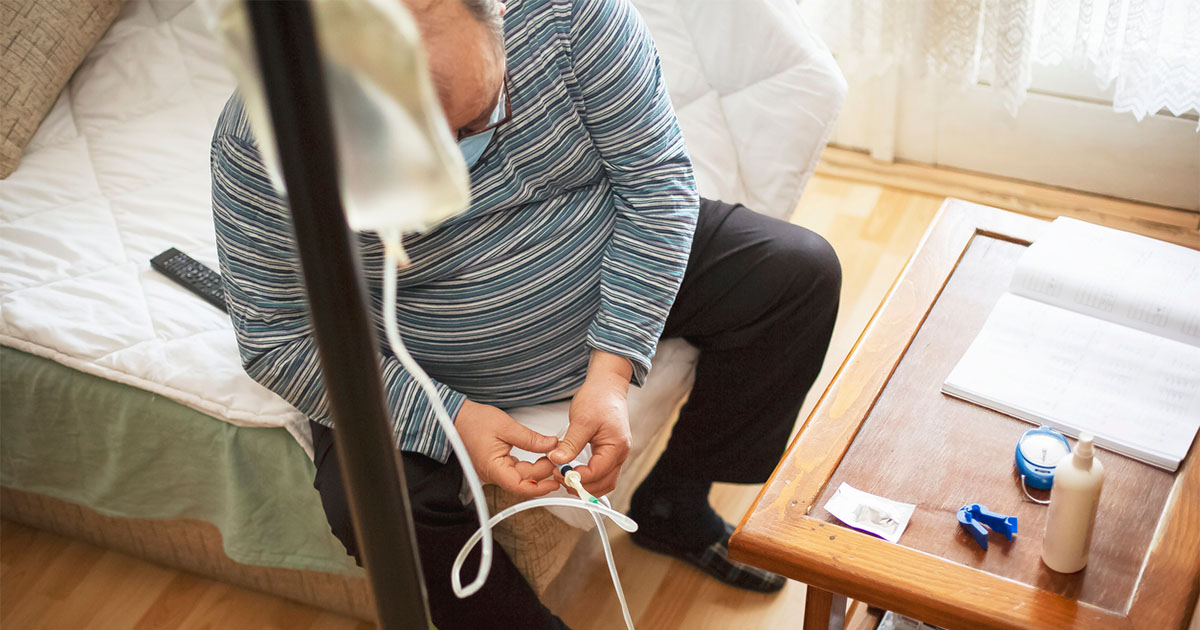
What was most important, and what becomes of major relevance when changing from oral medication to insulin, was the risk of hypoglycaemic attacks if too much insulin was administered. Initially I did check my blood glucose very regularly to establish a pattern. After a while I became more confident and began to have an awareness of when my blood glucose was rising or falling. I now check my blood glucose four times a day and record the level to establish a routine. The new meters are much faster now and more user-friendly, which is also an inducement to regular testing. Maintaining a regular regimen of activity does help to even out any peaks and troughs, but if I decide on physical activity such as walking or gardening then I increase my intake of carbohydrates to compensate. I also carry some form of carbohydrates with me for emergencies and also some form of medical card or identification in case of a hypoglycaemic attack, which may lead to a coma.
I have had a number of hypoglycaemic attacks since starting insulin treatment, most of which have been local to my home and easily redressed. There are times, however, when the attack happens and you are caught unawares. On one occasion when driving home from holiday I encountered grid-lock on the motorway only a few miles from the service station. I had carbohydrates in the car but was very concerned as to how long we might be stranded without assistance. Fortunately the traffic did free itself and I was able to make it to the service station safely. On anther occasion I had been to an exhibition at the National Exhibition Centre and despite eating well throughout the day I experienced an attack on the train returning home. The train did not have any buffet service and I had to assess my ability to make my destination without food. On this occasion I did suffer a bad hypoglycaemic attack and had to be taken home by friends, who at one point thought about driving me to the hospital instead.
Finding the right medication
I have now been through the learning curve of balancing my insulin with food intake and exercise and the risk of becoming hypo- or hyperglycaemic has lessened. I did find an exception, however, with the first type of insulin that I used. I was initially prescribed a mixture of rapid- and slow-acting insulin in the proportion of 70/30 in pre-mixed cartridges. At first this suited me and did the job, but soon I found that I was having hypoglycaemic attacks at night and sometimes during the day. If I needed to increase my dosage because of high blood glucose, the rapid-acting insulin brought my level down but at the same time this led to a build-up of the slow-acting insulin, which then caused me to become hypoglycaemic many hours later. There was a resultant yo-yo effect as I ate carbohydrates to cancel the hypoglycaemia and often took more insulin to counter the raised blood glucose level.
It was at this stage that I changed to taking a slow-acting insulin (glargine) once a day and rapid-acting insulin three times a day during or before meals. Very quickly my glycaemic level returned to a more stable level and remained very constant and controlled without the need for any more injections than I was already taking. I keep the dosage of the slow-acting insulin glargine constant and vary the rapid-acting dosage according to my glucose level, physical activity and food intake. This form of insulin was not available to me when I first started insulin treatment but has proved ideal and reliable.
Coping with restrictions and complications
I have now adapted to a way of life in which administration of insulin on a regular basis is a necessity and I know that there are wider implications of the regimen. When I changed to insulin as a form of medication I experienced sensory neuropathy in my hands and feet, a condition which has stayed with me and restricts the way in which I carry out my work and daily routine. I no longer climb or work at heights as this is a requirement of the Health and Safety Executive and a recommendation of Diabetes UK.
Support
Family and friends quickly realised my needs and restrictions which makes life easier and most organisations appreciate the needs of people with diabetes thanks to the good work of Diabetes UK and associated charities.
Managing now and in the future
The progress of my condition has now levelled thanks to my new insulin (glargine), and the guidance offered by my consultants, specialist nurses and dietitians at the diabetes clinic. As a result the future is more predictable and the inconvenience of injecting four times daily has become routine and part of my life. Having been through this learning curve of the transition from oral medication to insulin, my advice to all people with type 2 diabetes who need to start injecting insulin is to concentrate on good glycaemic control, healthy diet and a sensible exercise regimen combined with regular visits to your diabetes clinic.


No strong support for weight cycling causing detrimental changes in body weight, body composition or metabolism, but many gaps in the research.
5 Jun 2026