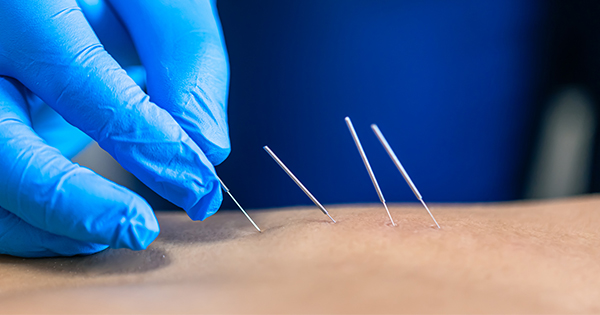
Peripheral diabetic neuropathy (PDN) is the most common complication of diabetes, and is a neuropsychiatric condition with myriad clinical manifestations (Hainline, 2011). Approximately one in three people with diabetes is affected by diabetic distal symmetric sensorimotor polyneuropathy and the condition is responsible for extensive morbidity, increased mortality, considerable interference with sleep, daily activities and an overall diminished quality of life (QOL). The early impairment of glucose handling, classified as prediabetes is also associated with neuropathy (Basić-Kes et al, 2011).
PDN is primarily symmetric sensory neuropathy, initially affecting distal lower extremities (Snyder et al, 2016). PDN manifests mainly as burning, pins and needles sensation starting in the feet and progressing upwards. The diagnosis excludes other aetiologies, commonly encountered in diabetics, such as neuropathies from alcoholism, vitamin B12 deficiency and uraemia, among others (Majid, 2010). Duby et al (2004) noted that the pathology of diabetic neuropathy involves oxidative stress, advanced glycation end products, pyolol pathway flux, and protein kinase C activation, all contributing to Microvascular disease and nerve dysfunction.
Treatment of PDN relies on the modification of the underlying disease and control of pain symptoms. The objectives of pharmacotherapy should be reduction of pain for maximum relief; balanced with acceptable side-effects and improvement in functional measures and QOL. Medication often fails to address any one of these objectives and patients often require more than one drug to provide adequate pain relief (Arora and Niraj, 2013). Potential drug interactions must be considered, given the frequent polypharmacy in people with diabetes; hence, the need for an individualised approach involving the patient in treatment selection.
Treatment is based on four cornerstones:
- Intensive diabetes therapy and multifactorial risk intervention.
- Treatment based on pathogenetic mechanisms.
- Symptomatic treatment.
- Avoidance of risk factors and complications (Ziegler et al, 2021).
Good glycaemic control is the priority for both prevention and management of PDN. However, even with good glycaemic control, up to 20% of patients will develop PDN and in the absence of treatment nerve damage may progress while pain diminishes (Corbett, 2005). PDN can lead to unfortunate limb loss and is the leading cause of lower limb amputation as 50% of PDN patients can be asymptomatic (Wooten, 2009).
Chao et al (2019) suggested that acupuncture therapy reduces pain from PDN and improves the QOL with no differences based on frequency of acupuncture. Acupuncture improves nerve conduction and clinical symptoms (Yu et al, 2021). It is hypothesised the mechanism may be related to the regulation of glucagon, activation of local blood circulation, relieving rigidity of muscles and activating collaterals (Ding et al, 2004). However, the results should be interpreted with caution owing to methodology flaws (Lin et al, 2021). Dimitrova et al (2018) reviewed trials of acupuncture and found acupuncture points used were closely associated with peripheral nerves and local needling is crucial for successful treatment of peripheral neuropathy.
Lai et al (2019) noted that acupuncture enhances the descending inhibitory effect and modulates the feeling of pain, thus modifying central sensitisation. There is an analgesic effect and a local reduction of inflammatory mediator levels. This improves the motor and sensory nerves function in patients with diabetic polyneuropathy; thus, acupuncture can be considered an appropriate safe and nonpharmacological complementary option for type 2 diabetic polyneuropathy.
Nash et al (2019) discovered improvements in PDN pain symptoms have been reported with benefit to improved sleep, fatigue, mood, function, QOL and ability to work (Andrew Moore, 2013) with no differences based on frequency (Chao et al, 2019).
Pain intensity is influenced by the meaning of the pain to the patient and its expected duration. Intensity is not the only factor important in the experience of pain; pain occurs within a context. For example, the environment also has an impact on the experience of pain, as do expectations, attitudes, and beliefs. Pain is rarely caused by psychological factors, but unfortunately diabetes is associated with psychological and emotional effects, such as fear, anxiety, and depression. This can lead to varying degrees of altered behaviour, dysfunction, or disability. This subjectivity recommends allowing the patient to report their symptoms; be it graphically or verbally.
The numerical rating scale (NRS) has been validated for the measurement of pain (Correll, 2011). It shows high reliability, good sensitivity, and concurrent validity in addition to generating data that can be statistically analysed for audit purposes (Jiang et al, 2021). Williamson and Hoggart (2005) found patients communicate far more information about their pain than just intensity; when using a pain rating scale. The NRS is preferred as a diagnostic tool for its simplicity and greater sensitivity to change. It is easy to administer and requires patients to assign a numerical score representing the intensity of their symptoms on a scale from 0-10 with 0 for having no symptoms and 10 having worst imaginable symptoms.
Aim
The aim of the study was to demonstrate the effectiveness of acupuncture therapy in reducing PDN to a manageable level and its usability as an alternative to drug therapy. No ethical approval was required due to the retrospective nature of the study.
Methods
Over a 6-year period, 114 patients were treated in an NHS clinic with acupuncture for PDN, There were 60 women and 54 men aged between 28 and 86 years. All patients who attended within this period and treated with acupuncture for PDN were included in this study. No patient was excluded. HbA1C was recorded alongside any diagnosed neurological conditions and if the patients were taking any medication to treat PDN. A 10 g monofilament was used to screen the foot for loss of protective sensation and DN4 neuropathic pain diagnostic questionnaire was used as a screening tool for neuropathy pain (Timmerman et al, 2017). Progress was recorded based on the patient’s reported improvement of symptoms using a NRS. Outcomes were measured by calculating the difference between the NRS at the first and final acupuncture session.
Individuals attended weekly sessions; the number of sessions ranged from one to nine. Each weekly session involved the insertion of six needles into each foot for 30 minutes. The six acupuncture points used were K1, KD5, KD7, medial and lateral approach to anterior ankle along joint line (ST41), between the first and second metatarsal (LV3), all needles stimulated to reach de qi. De qi is the descriptive nature of the sensations felt by the patient and often described as a dull ache or tingling feeling (Joyce et al, 2016).
Additionally, advice was provided concerning the poor management of blood glucose. The NRS was used at every appointment where acupuncture was provided. These results were then analysed to determine if patients reported a reduction of pain using the NRS comparing the NRS at the start of the acupuncture therapy and the final session of acupuncture.
Statistical analysis
Statistical analysis was performed using SPSS statistics software (version 22.0; SPSS, Chicago, Illinois, US). Statistical significance was defined as P<0.05. Changes in the NRS following treatment were analysed using a two-tailed paired t-test. Relationships between continuous variables were analysed using univariate and bivariate statistics. A Point-Biserial correlation was used to review relationships between having a pre-existing neurological condition and changes in NRS.
Results
A total of 114 patients (60 women and 54 men) seen over a 6-year period between 2016 and 2022 were included. The mean (SD) age was 64 years (12). Patients received a mean (SD) 4 (1) sessions of treatment. Fifty (44%) patients had a neurological disorder prior to treatment. Further details of associated neurological conditions are given in Table 1.
The mean (SD) HbA1c prior to therapy was 75 (21). At the start of therapy, the mean (SD) NRS was 8.6 (1). Following completion of therapy, the mean (SD) NRS was 4 (3) with a mean (SD) difference of 4.7 (3) (P<0.01) (Figure 1). There was no association between HbA1c (at the start of therapy) or existence of another neurological condition with changes in the NRS (P=0.5 and P=0.6, respectively). Finally, there was a significant relationship between number of sessions and decrease in NRS. The greater the number of sessions, the greater the reduction in the NRS (r=0.5, P<0.01; Figure 2). However, clinical acupuncture practices vary greatly and leads to different choice of acupuncture points and duration by each clinician; these are mainly based on clinicians’ personal experience.
Discussion
Research regarding methodology of acupuncture for the treatment of PDN is sparse with duration and frequency varying extremely. Variations were found in needle retention time and point selection, as well as a total number and frequency of treatments (Jeon et al, 2014; Bailey et al, 2017). Due to time constraints patients in this study were offered five sessions initially but some requested more sessions of acupuncture and some attended for fewer than five sessions. However, there was a significant relationship between the number of sessions of acupuncture and the reduction in NRS.
Chao et al (2019) observed no significant differences between once/twice weekly acupuncture. Compared with usual care, participants randomised to acupuncture experienced greater decreases in pain during the 12-week intervention period, but benefits were not maintained after acupuncture ended; however, QOL improved. Further research and follow-up post acupuncture therapy would prove useful to explore the effectiveness of acupuncture long term.
Abuaisha et al (1998) delivered six courses of classical acupuncture analgesia over a period of 10 weeks. The study showed significant improvement in primary and/or secondary symptoms. Patients were followed up for a period of 18–52 weeks, with 67% of subjects able to stop or reduce their medications significantly.
Nash et al (2019) found acupuncture for PDN appeared to improve symptoms and the most common acupuncture point selections were ST36 and SP6, but half the studies they reviewed used local point selection. The six acupuncture points used in their study were traditional acupuncture points surrounding local nerves. However further research is required to explore the effectiveness of traditional acupuncture point selection versus local point selection.
Garrow et al (2014) found that acupuncture was well-tolerated, with no appreciable side-effects. Ahn et al (2007) reported similar results. They found traditional Chinese medicine acupuncture lowered pain according to the McGill Short Form Pain score and reported an improvement in nerve sensation according to quantitative sensory testing.
Youssef et al (2022) reported that the acupuncture group showed significant increase in nerve conduction velocity of tibial and sural nerves in both sides post treatment compared to pre-treatment.
Acupuncture has a significant effect on improving sensory perception combined with motor and sensory nerve function and conduction in patients with diabetic polyneuropathy (Schroeder et al, 2008; Dimitrova et al, 2017). Exploration of improved sensation post acupuncture therapy would be beneficial to diabetic patients and the impact of neuropathy on the QOL.
Wei-jing et al (2021) used descriptive analysis to show significant improvement in PDN symptoms, accelerate the conduction velocities of sensory and motor nerves, and up-regulate the content of plasma nitric oxide, while the adverse reaction rate was low.
Tong et al (2010) found three of the six measures of motor nerves and two measures of sensory function demonstrated significant improvement over a 15-day treatment period. They found acupuncture was significantly more effective than sham for treatment of numbness of the lower extremities, rigidity in the upper extremities and alterations in temperature perception in the lower extremities after therapy.
Zhang et al (2010) found a total effective rate of 85.5% with acupuncture. Likewise, our results also showed a reduction in 4 points on the NRS for PDN, a significant reduction in the intensity of pain.
Tong et al (2010) found acupuncture was significantly more effective for treatment of numbness of the lower extremities, spontaneous pain in the lower extremities, rigidity in the upper extremities, differences in vibration perception threshold and alterations in temperature perception in the lower extremities. Ahn et al (2007) also reported improvement in nerve sensation according to quantitative sensory testing; however, claims mechanism of action remains speculative. Meyer-Hamme et al (2021) presumed the significant improvements in Nerve Conduction Studies values indicates structural neurogeneration following acupuncture. Acupuncture showed significant improvement in PDN symptoms (Cho and Kim, 2021; Jeon et al, 2014) and may be considered an appropriate safe and non-pharmacological complementary treatment option for type 2 diabetic polyneuropathy (Jung and Chen, 2013).
Future directions
Acupuncture has been demonstrated as a practical and feasible treatment modality for people with PDN. Potential problematic issues surrounding acupuncture treatment for PDN are low-quality evidence, unitary outcome measures, poor methodological quality of systematic reviews and nonstandard reporting (Wei-jing et al, 2021).
Lin et al (2021) carried out a study to evaluate the methodology quality of systematic reviews regarding acupuncture for PDN. They recommended all results of any studies looking at the use of acupuncture therapy for PDN should be interpreted with caution owing to methodology flaws. Bo et al (2012) found the quality of the reports on RCTs of acupuncture for PDN is moderate to low.
There is a need for larger randomised trials to confirm the clinical effectiveness and cost effectiveness of acupuncture combined with an evidence-based approach to provide greater confidence in its use (Garrow et al, 2014; Yu et al, 2021).
Conclusion
This retrospective study demonstrated the effectiveness of acupuncture therapy in the reduction of peripheral diabetic neuropathy pain to a manageable level using the NRS; and an increase in acupuncture sessions showed further improvement. It highlights the need for further research into alternative therapy for a population that is reliant on drug therapy and suffering the associated side-effects.