General changes
● Language changes: Person-first, culturally sensitive and inclusive language; terminology designed to empower people.
Section 1. Improving care and promoting health in populations
● Additional cost data, particularly regarding insulins and glucose monitoring technology. For UK prices, consult BNF or Summary of Product Characteristics.
Section 2. Diagnosis and classification
● More structured approach to diagnostic testing including confirmation of initial diagnosis, with a focus on HbA1c use.
● Standardised islet autoantibody testing to help differentiate classification.
● Screening recommendations in those treated with second-generation antipsychotic drugs, those with acute or chronic pancreatitis, and those with cystic fibrosis.
Section 3. Diabetes prevention
● Monitor people at risk of developing type 1 diabetes. Teplizumab recommended to delay onset of stage 3 (symptomatic) type 1 diabetes in people aged 8 years or older with preclinical (stage 2) type 1 diabetes.
Section 4. Medical evaluation and comorbidities assessment
● Immunisations: Added respiratory syncytial virus vaccine in adults aged ≥60 years.
● Bone health: Extensively revised/updated – regular review, identification and management. New Table 4.5 summarises fracture risk factors.
● Liver disease: 2023 “Living Standard” changes incorporated, including screening and management recommendations. Proposed nomenclature changes (metabolic dysfunction-associated steatotic liver disease; MASLD) discussed but not implemented.
Section 5. Positive health behaviours
● Focus on guiding healthcare professional behaviour rather than patient behaviour.
● Five critical times to evaluate need for structured diabetes education: diagnosis; not meeting treatment targets; annually; when complicating factors (medical/physical/psychosocial) develop; transitions in life and care.
● Medical nutrition therapy: Updated general diet guidance for diabetes, healthy fats, religious fasting, chrononutrition, non-nutritive sweeteners (based on 2023 WHO guidance).
● Physical activity: Updated to define sedentary behaviour, benefits of high-intensity training.
● Smoking cessation: Ask and refer. Cannabis discussion added.
● Implement psychosocial screening protocols consistently (for diabetes distress, stress, quality of life, financial/social/family/emotional resources, psychiatric history, depression, fear of hypoglycaemia).
● Encourage sleep-promoting routines.
Section 6. Glycaemic goals and hypoglycaemia
● Hypoglycaemia guidance consolidated here from other sections.
● Discussion of strengths and limitations of HbA1c and other glycated proteins.
● CGM metrics added to glycaemic goals section.
● Deintensification of medication added.
● Increased focus on assessing, preventing and managing hypoglycaemia risk, awareness and hypo education.
Section 7. Technology
● Clinicians to upskill as required to assist with devices and technology.
● Recommendations reflecting benefits of CGM and automated insulin devices for additional groups.
Section 8. Obesity and weight management
● Importance of weight management in diabetes; benefits gained by different weight loss achievements.
● Use BMI and measures of body fat distribution (e.g. waist circumference, waist:hip ratio, waist:height ratio).
● Individualise management; consider all approaches (behavioural, pharmacological, surgical).
● Weight maintenance programmes recommended for those who achieve weight loss.
● Effective GLP-1 or GIP/GLP-1 receptor agonists (i.e. semaglutide, tirzepatide) recommended as pharmacotherapies of choice.
● Emphasis on re-evaluating treatment, goals and preventing therapeutic inertia.
● Consider long-term benefits of surgery, monitor post-surgery weight loss and explore barriers and additional interventions if needed.
Section 9. Pharmacological approaches to glycaemic treatment
● Analogue (or inhaled) insulins preferred for most with type 1 diabetes to minimise hypoglycaemia.
● Consider glucagon (preferably ready-to-use) for those taking insulin or at high risk of hypos.
● Consider early combination therapy in type 2 diabetes to shorten time to achieving treatment goals.
● Intensify treatment to achieve glycaemic and weight loss goals in people with type 2 diabetes and no CVD/CKD comorbidities. Individualise choices and prioritise drugs which reduce CVD, heart failure and CKD.
● GIP/GLP-1 receptor agonists added as options alongside GLP-1 receptor agonists for treatment escalation, in preference to or in combination with insulin.
● Consider insulin at any stage in individuals who need it, but adjust doses of other glucose-lowering medications if hypo risk.
Section 10. Cardiovascular disease
● Bempedoic acid recommended as an option for primary prevention in statin-intolerant people. Bempedoic acid, PCSK9 inhibitors and inclisiran recommended as alternative/additional lipid-lowering therapies if intolerant or not meeting targets. New subsection on Statin Intolerance.
● Screen for asymptomatic heart failure in people with diabetes using BNP or NT-proBNP.
● Screen for asymptomatic peripheral arterial disease using ankle–brachial index if age ≥50 years, any microvascular disease, foot complications, diabetes end-organ damage and in those with diabetes of ≥10 years’ duration.
● Use SGLT2 or SGLT1/2 inhibitors if diabetes and established heart failure (all types).
● If using SGLT2 inhibitors, educate on risks and signs of ketoacidosis in type 1 or ketosis-prone diabetes, and if eating ketogenic diet (other guidance recommends this for everyone taking SGLT2 inhibitors).
Section 11. Chronic kidney disease
● Updated to align with 2023 ADA and KDIGO consensus on diabetes management in CKD 2023, including CKD progression, monitoring and referral recommendations.
● ACE inhibitors or ARBs recommended in people with uACR 30–299 mg/g (approximately 3–30 mg/mmol) and strongly recommended in those with uACR ≥300 mg/g (30 mg/mmol) and/or eGFR <60 mL/min/1.73 m2, to slow renal progression and reduce cardiovascular events.
Section 12. Retinopathy, neuropathy and foot care
● Updated to include use of FDA-approved AI algorithms to analyse retinal photography to improve access to screening; importance of evaluation and rehabilitation of visual loss.
● Limited evidence for lidocaine 5% plasters/patches for neuropathy pain and gastric stimulation for gastroparesis.
● Specialist multidisciplinary management for those with foot ulcers and/or high-risk feet.
Section 13. Older adults
● Individualise glycaemic goals due to heterogeneity of older people with diabetes. Stronger recommendations made to deintensify/switch to medications with lower hypoglycaemia risk.
● Emphasis that older people with comorbidities should be offered drugs that improve cardiorenal outcomes, irrespective of glycaemia.
Section 14. Children and adolescents
● Diagnose and manage psychosocial needs.
● Comprehensive lifestyle intervention aiming for at least 7–10% weight loss.
● Empagliflozin added to the list of agents recommended for treatment escalation in children and young people aged ≥10 years.
● Discourage starting smoking and encourage cessation.
Section 15. Pregnancy
● Glucose monitoring updated to include recommendation for CGM in women with type 1 diabetes and consideration in those with type 2 or gestational diabetes.
● Metformin and glyburide not to be used first-line.
● Aspirin for pre-eclampsia to be considered in gestational diabetes if single high risk factor or multiple moderate risk factors.
● Encourage breastfeeding for all with diabetes.

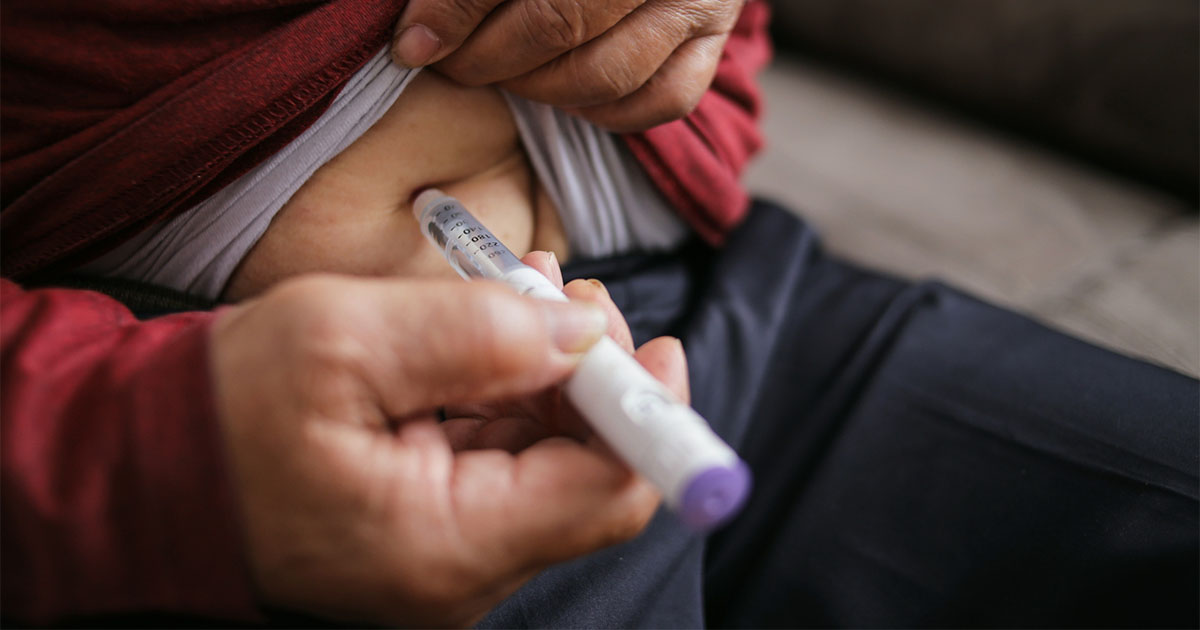
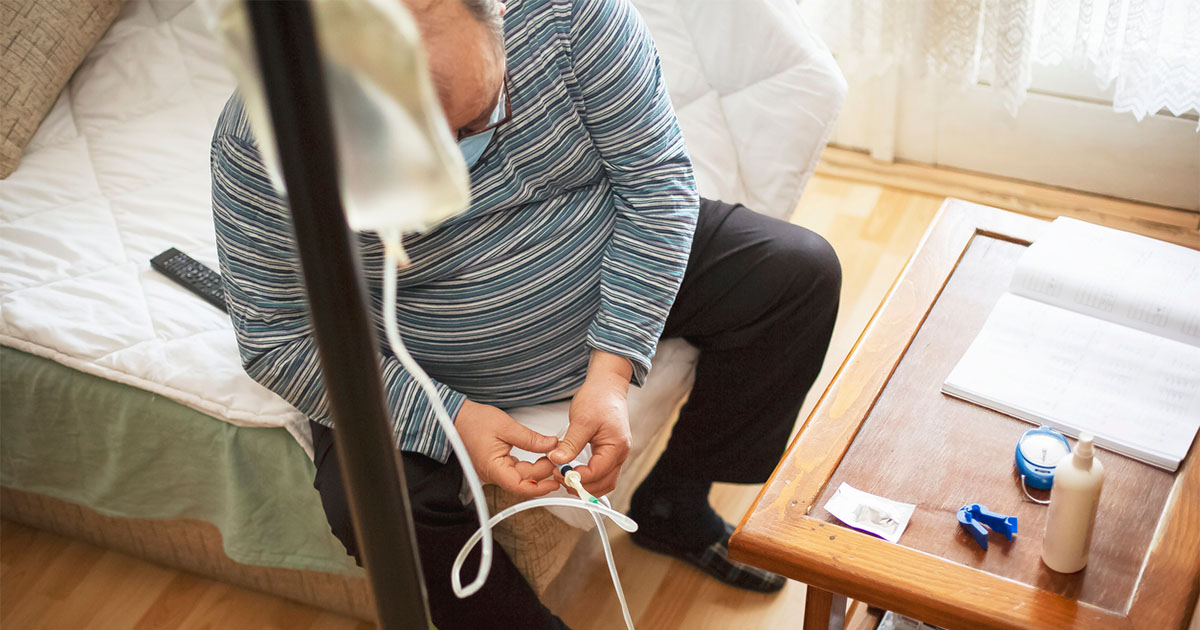


No strong support for weight cycling causing detrimental changes in body weight, body composition or metabolism, but many gaps in the research.
5 Jun 2026