Globally, diabetes is one of the four most common non-communicable diseases (World Health Organization [WHO], 2020). Serious complications, such as loss of eyesight and compromised sensation and circulation in the lower limbs, are associated with poor control of the condition (Ruston et al, 2013).
Diabetes is one of the few chronic conditions that can be largely self-managed by the people living with it (American Diabetes Association [ADA], 2020) and, in view of the time spent by individuals at their place of employment, the management of their condition whilst at work is very important.
Background
Research about diabetes and employment is limited and predominantly quantitative in nature (Tunceli et al, 2005; Herquelot et al, 2011; Breton et al, 2013; Stynen et al, 2015; Kouwenhoven-Pasmooij et al, 2016), with only one qualitative study (Ruston et al, 2013). To date, the evidence suggests that diabetes negatively impacts the workforce in terms of early retirement, sickness absence, disability benefits and productivity (Ruston et al, 2013).
Methods
Aim
The aim of the study was to explore the support and challenges experienced by adults living with diabetes in fulfilling their respective employment commitments.
Design
A qualitative exploratory approach using one-to-one interviews was adopted. Thematic analysis was used to analyse the data (Miles et al, 2014). Participants were purposively selected, and triangulation of data sources was employed for thoroughness and not for confirmation purposes (Adami and Kiger, 2005). The inclusion criteria applied for employees were:
- Employed in their current place of work for a minimum of 6 months.
- Diagnosis of diabetes for at least 2 years.
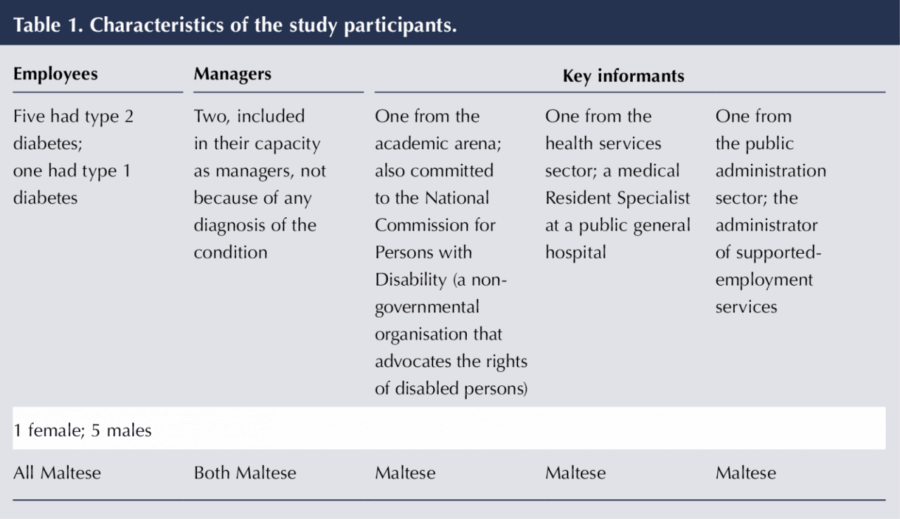
The sample consisted of six employees and two managers of an organisation based in Malta, plus three key informants whose roles comprised clinical duties, employment duties and advocacy related to persons with chronic conditions. Selection of the key informants was purposive and drew upon their commitment. Their contribution was to provide perspectives that went beyond the data collected from the employees in their interviews. Table 1 shows the sample characteristics of the whole group.
Data collection
Semi-structured, face-to-face, individual interviews were conducted with all the participants. The interviews with the employees were held at the doctor’s clinic within the organisation itself, whereas those with the managers and key informants were held at their work offices. The maximum interview duration was 90 minutes. Each was audio recorded with the permission of the participants. Only the researchers had access to the full recordings and transcripts, and confidentiality was ensured throughout.
Ethical considerations
The study was approved by the University Research Ethics Committee of the University of Malta. The employees were recruited via the company doctor, whereas the managers were recruited through the human resources (HR) management. The company doctor and the HR management provided potential participants with written information, and signed consent was sought prior data collection.
Data analysis
The interviews were transcribed by the researcher and thematic analysis of the transcribed data was carried out in keeping with Miles and Huberman’s model (Miles et al, 2014).
Findings
Analysis of the data elicited three themes: (i) Awareness of the complications and risks associated with diabetes; (ii) working with diabetes; and (iii) services and initiatives that support employees. Each of these themes is explored below.
Discussion
Awareness of the complications and risks associated with diabetes
The majority of the employees demonstrated awareness of the complications of diabetes and of the importance of regular monitoring to delay them, as illustrated by these quotes:
“Let me explain, I am fully aware that some complications might lead to leg amputations. I try to exercise control and attend each and every appointment.” (P2)
However, the findings suggest limited understanding of the seriousness of these complications. For example, one participant said:
The data appear to reveal the challenges associated with inadequate health literacy. Health literacy is not merely the ability of an individual to read health-related information or to organise indicated health appointments, but is evident when it leads to the empowerment of an individual (WHO, 2016). This study suggests a gap in employees’ and managers’ health literacy and, therefore, limited empowerment.
When asked whether the complications of diabetes created problems in the world of employment, both the medical sector and the supported employment sector key informants claimed that they were not aware of such instances. However, the key informant from the academic sector showed some concern with respect to employees not giving their 100% at work due to this chronic condition. The findings of one research study suggest that the effect of the symptoms and complications of diabetes often hinders employees from being fully productive at their workplace, and that this might even result in these employees leaving the workforce (Rumball-Smith et al, 2014). It quotes another study that states that the complications that may arise from diabetes can be so significant that a person might stop working for good or significantly increase the number of sick-leave days they take (Tunceli et al, 2005).
Working with diabetes
All six employees claimed to manage their condition very well at their place of employment and that it rarely interferes to any significant extent with their day-to-day work. According to the ADA (2014), diabetes is highly unlikely to impose substantial impacts on the ability of the individual to pursue a particular career; in fact, more often than not, the employer is unaware of the employee’s condition.
The employees did not identify any major challenges attributed to diabetes at their place of work, though fear of hypoglycaemic episodes at work did persist.
The managers both claimed that they were not aware that their employees experience any particular challenges with diabetes whilst working. Similarly, the key informants noted that, to the best of their knowledge, employees with diabetes cope well at their workplace. They believed that diabetes does not impose major challenges in employment.
However, Stynen and colleagues (2015) found that significant challenges are associated with diabetes and that employees with diabetes are, in fact, vulnerable to losses in particular domains of functioning (i.e. need for recovery, restrictions in social participation and physical demands), which may lead to early retirement. The fact that the employees and managers did not point out any particular challenges in the present study could be attributed to them not being aware of certain challenges and, thus, not perceiving them as such. A clear example is certain participants’ lack of awareness regarding the importance of maintaining rigid control of lifestyle and strict glycaemic control. This is consistent with research that found that employees often undervalue the magnitude of the challenges inherent in managing diabetes in the workplace (Ruston et al, 2013).
Work environment and nature of job
Despite the majority of participants not identifying any major challenges in relation to their diabetes in the workplace, some did mention factors that influence the management of their condition. One employee said:
“I regularly have to travel to different departments, which are far from each other, leaving often little time for me to eat, thus risking a low blood glucose level.” (P3)
Regarding managers not being adequately aware that the work environment could be impeding optimal management of their employees’ chronic condition, the findings of our study are similar to those of Ruston and colleagues (2013). The ADA (2014) states that the employer should always evaluate the safety risks of employees with diabetes, echoing the work of the theorist Abraham Maslow (1943) who identified safety as being the most important element of employment.
Support at work and flexible break hours
None of the employees interviewed were aware of any support services specifically for employees with diabetes being offered by the organisation, besides the services provided by the company doctor. Nonetheless, the participants explained that the organisation accommodates their chronic condition by “bending its rules as needs be”. An employee said:
According to the ADA (2014), several things can be done by an employer to further facilitate the lives of employees with diabetes. These include allowing time and an adequate place for blood glucose monitoring and administration of insulin (if applicable), and easy access to food and beverages whenever the employee feels it is necessary. It also suggests flexible breaks and shift patterns that can accommodate the multiple medical appointments that they need to attend.
Emphasising normality
In this sub-theme, an employee commented on how he feels like a completely normal person despite his diabetes. This point was also emphasised by one of the managers, who said that employees with diabetes are like all the rest. Ruston and colleagues (2013) proposed the need to protect and foster normality in employees who have diabetes.
The key informant from the supported employment sector provided an alternative viewpoint. The Convention on the Rights of Persons with Disabilities (United Nations, 2007) states that everyone has the right to employment on an equal basis, provided that they are equipped with the necessary education. She pinned her contribution to this convention, and emphasised that the employer should fill a job position as required and address the situation accordingly. She supported pre-employment medical tests and stressed the importance of the employee being honest regarding their medical condition. This is consistent with the literature, which advocates disclosure with employers regarding diabetes (Ruston et al, 2013).
Managers identified the company’s annual Wellness-Being Week (a week-long education initiative for all staff) and gym membership offers, special time out, health insurance coverage and access to kitchenettes as corporate initiatives that support employees with diabetes.
Evidence suggests that managers know little about the chronic conditions that their employees suffer from or about the impact that the work environment has on the ability of these employees to manage their condition at work (Ruston et al, 2013). The same study found that employees expect very little support from their employers. Collectively, the evidence highlights the importance of educating and supporting people to disclose their condition and to seek the necessary support at their place of work. Ruston and colleagues (2013) also suggested that organisations are more likely to experience an increased loss of productivity and absenteeism if their employees’ needs are neglected, a finding also noted in other studies (Tunceli et al, 2005; Breton et al, 2013; Rumball-Smith et al, 2014; Stynen et al, 2015). The evidence highlights the significance of health-management strategies that are work-based.
Services and initiatives that support employees
Employees showed minimal interest and shared very limited ideas regarding the initiation of new services to help them with their working lives. The findings of this research study concur with another (Ruston et al, 2013), in which employees stated that managing their condition at the workplace was solely their responsibility, and that it was also their duty to bring with them whatever resources were necessary and to engage in whatever action was needed to manage their condition.
One manager claimed that he does not see the need for any new services or initiatives to be implemented, as diabetes has never caused any problems at the workplace. On the same lines, the other manager stated that what was already available, even in terms of services provided by the company, was adequate. Nevertheless, he suggested the introduction of a wider selection of healthy food options at the staff canteen.
Both the employees and employers being satisfied with the situation concerning the services being offered towards employees with diabetes could be related to gaps in health literacy. Cavanaugh (2011) explains how health literacy is directly related to the prevalence of diabetes and its management by the person who has the condition. The debate over whether it is the duty and responsibility of managers to enhance the health literacy of their respective employees is unresolved. One questions whether health literacy can be actively enhanced in everyone, and whether health literacy is influenced by factors that are, in turn, influenced by the managers themselves, such as immediacy of access to information.
Limitations of the study
The main limitation of this study is that the participants were chosen from only one organisation. This jeopardises the generalisability and transferability of the data, but transferability was not the scope of the research. Also, the researcher was not a diabetes health specialist and did not work in a clinical area dedicated to diabetes care. This may have jeopardised critical analysis of the data.
Conclusion
Through this study, the researcher explored the support and challenges experienced by adults with diabetes in fulfilling their employment commitments. It is hoped that the findings will contribute towards the enhancement of employees’ experience with diabetes at their place of work and, in parallel, may inform employers and guide policy development. The clinical implications of the findings include the need for diabetes nurses in the employment sector. They may be best equipped to guide and support the development and delivery of targeted services for employees with diabetes. Moreover, diabetes nurses are best suited to empower employees, alongside heightening the level of health literacy of both employees and managers. Aligning managerial decisions and operational processes to the needs of employees with diabetes is a central exercise that diabetes nurses may address effectively.
Relevance to practice
Job applications from people with diabetes should be evaluated on a case-by-case basis in view of the reasonable adjustments in the workplace that may be indicated owing to the applicant’s chronic condition. The need for reasonable adjustment in this regard must not translate into any discrimination towards the applicant. Minor adjustments in the workplace, such as flexible break-times, accessible kitchenettes and private areas for the administration of medication, can be very effective in supporting employees with diabetes. Policymakers should address the need for measures to ameliorate the working lives of such employees in a more focused manner, and be aware that measures to support employers, such as targeted grants towards initiatives, are also indicated.
Relevance to education
People with diabetes and employers should receive better education on what it means to work with diabetes and what needs to be done to support their employment. Most self-management education programmes focus on how to manage the condition whilst at home, but it is recommended that a portion of such programmes cover other environments. Education of the wider public on what it means to have diabetes and to work with such a condition is advisable to address some prevailing attitudes that may be unhelpful, and could help confront discrimination when individuals with diabetes apply for jobs (Malta Ministry for Health, the Elderly and Community Care, 2010). Furthermore, it is suggested that frequent educational sessions are run at all organisations to further enhance the management of diabetes, improve awareness of possible serious long-term complications, prevent the onset of new cases and foster understanding and cooperation amongst employees. The findings of this study also shed light on the training needs of healthcare professionals.
Recommendations for research
More qualitative studies should be conducted with a focus on the day-to-day activities and management at the place of employment. Future studies need to span different types of employment entities, spanning the private and public sectors.





Helping homeless adults to overcome the challenges of managing their condition.
16 Apr 2024